
As cycling is a very repetitive sport, any injuries that occur tend to be related to overuse and can usually be attributed to inadequate bike setup, training volume...
Learn More
How Technology like Hand-held Dynamometry is Changing Recovery Technological innovation is rapidly reshaping healthcare—and physiotherapy is no exception. One of the most significant advancements in recent years is...
Learn More
Our bones make slight changes to their architecture every day. This process is called remodelling and it occurs in response to the pressures and forces we put on...
Learn More
Sports injury prevention physiotherapy focuses on building strength, managing training load, prioritising recovery, and addressing early warning signs before minor issues become significant injuries. Research supports progressive strength...
Learn More
Why Real-Time Ultrasound Is a Game-Changer for Muscle and Joint Health Real-Time Ultrasound (RTUS) has emerged as an innovative, highly effective tool in physiotherapy, transforming the way we...
Learn More
A pain in ones foot can start off as a small discomfort but after a day of walking, jogging, or even standing in high heels, a small issue...
Learn More
Why Clinical Pilates is Perfect for Every Body Clinical Pilates is a fantastic option for exercise based rehab, as it offers a tailored, evidence-based method to help individuals...
Learn More
Sports Injuries: Prevention, Recovery and Performance Sports injuries affect people of all ages, fitness levels, and abilities. While athletes often perform at higher levels of strength and function,...
Learn More
How Pre and Post-Operative Physiotherapy Prepares Your Body for Surgery Introduction Undergoing surgery is a significant event, and ensuring your body is well-prepared can make a remarkable difference...
Learn More
Osgood-Schlatter Disease Osgood-Schlatter Disease is a common condition that affects the knees, primarily in adolescents, particularly during growth spurts. It is characterised by pain, swelling and tenderness just...
Learn More
What is Osteoporosis? Osteoporosis is a medical condition diagnosed in individuals with low bone mineral density. The current definition is those with bone mineral density that is greater...
Learn More
Keith recently attended the Sporting Hamstring course conducted by Geelong Cats head physio Mark Young and AIS track and field physio Ben Raysmith and provides insight into how...
Learn More
Total knee replacement (TKR) ranks among the most commonly performed orthopaedic surgeries, with over 50,000 procedures annually in Australia. This figure is projected to rise substantially in the...
Learn More
The Benefits of Physiotherapy for Seniors: Stay Strong, Mobile and Independent As we age, our bodies change – but that doesn’t mean strength, mobility or independence are out...
Learn More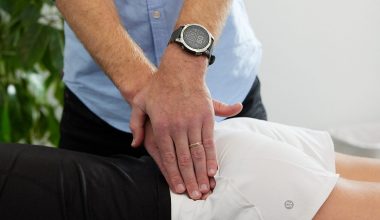
Understanding Australia’s Most Common Physiotherapy Conditions: What We See Every Day As physiotherapists here at Malvern Physiotherapy Clinic, we’re often asked about the types of conditions we treat...
Learn More
You may have heard about Pilates from a friend or even had a recommendation from your doctor. Pilates has gained immense popularity over the years. It offers a...
Learn More
What is it? The fascia is a tough, fibrous connective tissue that supports the arch of the foot and transmits forces. It’s intricately attached to the heel, toes,...
Learn More
An ankle sprain is one of the most common injuries affecting the foot and ankle, particularly during sport or when walking on uneven ground. It occurs when the...
Learn More
Understanding Inflammation: What It Is and How Physiotherapy Can Help Inflammation is a natural response in the body, playing a crucial role in healing and recovery. However, when...
Learn More
One of the most common misconceptions when working with a physio is that your treatment is limited to your appointment. In fact, one of the most crucial elements...
Learn More
The Essential Role of a Specialist Physiotherapist in Your Rehabilitation When recovering from an injury or managing a complex musculoskeletal condition, expert care can make all the difference....
Learn More
Discover everything you need to know about physiotherapy, what physiotherapists do, how they help, and when you should seek advice from a physio. Our warm and friendly team...
Learn More
If you’ve suffered a soft injury in the past – even a garden variety strain or sprain – chances are you’ve been advised to use the RICE method...
Learn More
Comparing Musculoskeletal and Sports Physiotherapy: Which One Do You Need? When seeking physiotherapy, it can be helpful to understand the different areas of expertise within the profession. While...
Learn More
Dry Needling vs. Acupuncture: Key Differences, Similarities, and Where They Overlap If you’ve ever explored options for managing pain, muscle tightness, or chronic conditions, you’ve probably come across...
Learn More
Chronic Pain and Physiotherapy: What You Need to Know Living with chronic pain can be exhausting. Unlike acute pain, which usually resolves as the body heals, chronic pain...
Learn More
Finding the Best Physiotherapy Near You: A Local Guide If you’ve ever searched “physiotherapy near me” online, you’re not alone. In Australia, thousands of people search this term...
Learn More
Relieve TMJ pain with expert physiotherapy at Malvern Physiotherapy If you’ve ever experienced pain, clicking, or difficulty moving your jaw, known as the temporomandibular joint or TMJ, you...
Learn More
How Real-Time Ultrasound Can Improve Muscle Activation Muscle activation is a critical component of effective rehabilitation. When muscles fail to activate correctly after injury, pain or surgery, recovery...
Learn More
One of the most influential recent developments in sports medicine’s understanding of human physiology has been grasping the effect that load has on tissue. When I speak of...
Learn More
Everybody will have experienced a time when they have an important event coming up, and the last thing they could possibly want is an injury. So, how can...
Learn More
Can Stretching Reduce Muscle Injury Risk? What the Evidence Really Says Flexibility exercises are often recommended to improve movement, reduce tightness, and support recovery. However, many people...
Learn More
Managing Common Health Concerns with Physiotherapy Physiotherapy is an essential part of allied health care, offering a hands-on and evidence-based approach to managing a wide range of health...
Learn More
Debunking Myths About Remedial Massage: How It Supports Pain Relief and Recovery Remedial massage is a powerful tool in managing pain, improving movement, and supporting recovery from...
Learn More
Pain on the side of your hip? It could be due to trochanteric bursitis. This is the inflammation or swelling of the bursa (fluid-filled sack) that sits in...
Learn More
Osteoarthritis is the breakdown and erosion of cartilage that overlies bone within a joint. This process results in inflammation within the joint, and is often felt as pain...
Learn More
Bursitis is commonly diagnosed as the cause of pain in many areas of the body; you may have heard of it when people discuss their shoulder or hip....
Learn More
Shoulder Pain Malvern: How Physiotherapy Can Help You Recover Shoulder pain can significantly impact your daily activities, from simple tasks like reaching overhead to more complex movements involved...
Learn More
Clinical Pilates: Strengthening Your Core for Injury Prevention Clinical Pilates is a highly effective, physiotherapist-led approach to improving strength, stability and movement control. At Malvern Physiotherapy Clinic,...
Learn More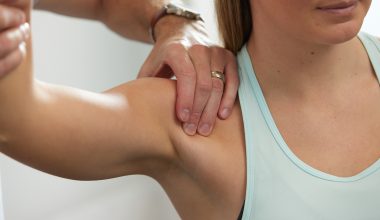
The shoulder is one of the most difficult joints to treat as it relies on many components to act in sync for correct function. We as humans are...
Learn More
What is Osteoporosis? Osteoporosis is a medical condition diagnosed in individuals with low bone mineral density. The current definition is those with bone mineral density that is greater...
Learn More
As the physical distancing measures are becoming the new normal, we are here to help you navigate this time with regards to your physical health. The emphasis from...
Learn More
“Core”…what does it even mean? The concept of “core” means different things to different professions. Core can refer to the abdominal muscles, pelvic floor muscles, the muscles that...
Learn More
Understanding Inflammation: What It Is and How Physiotherapy Can Help Inflammation is a natural response in the body, playing a crucial role in healing and recovery. However, when...
Learn More
Running technique has become a hot topic recently with a growing trend towards ‘barefoot’ running and forefoot strike. The popular book “Born to Run” by Christopher McDougall along...
Learn More
Keith recently attended the Sporting Hamstring course conducted by Geelong Cats head physio Mark Young and AIS track and field physio Ben Raysmith and provides insight into how...
Learn More
Finding the Best Physiotherapy Near You: A Local Guide If you’ve ever searched “physiotherapy near me” online, you’re not alone. In Australia, thousands of people search this term...
Learn More
Congratulations to all those who participated in the Nike Melbourne Marathon Festival this past weekend. Runners of all ages and abilities came together to push their limits and...
Learn More
A UK study found that at least ¼ of those aged over 55 years of age suffered persistent knee pain each year. A Finnish paper also found knee...
Learn More
Posture is a frequent topic of discussion for physiotherapists at Malvern Physiotherapy Clinic, clients, the media and society. A common belief is that spinal pain is caused by...
Learn More
INJURY PREVENTION – Have you ever suffered pain that has limited your function so much you’re your only focus has been to escape this pain? Then once the...
Learn More
All the joints in the body have the capacity to make noises, some of which are a cause for concern, others are non sinister things happening within the...
Learn More
The start of the new school year has arrived and as a parent you want to ensure your child has the best possible experience. One important aspect is...
Learn More
Strength training is typically seen as a way to mould, shape and develop the human body. It achieves these changes through controlled loading of muscle, tendon and bone...
Learn More


